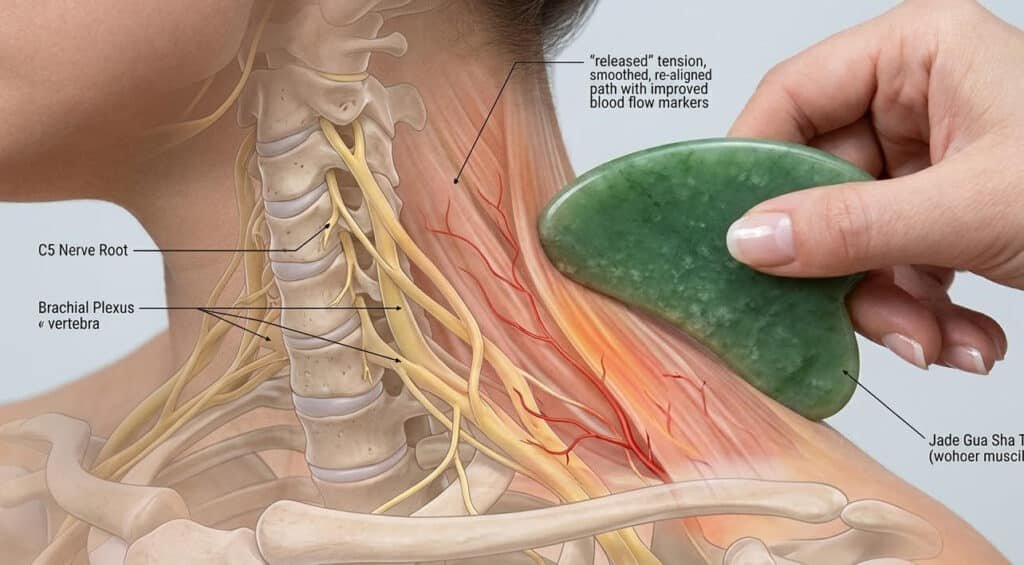
The question most people ask is straightforward: can massage help a pinched nerve? The short answer, backed by peer-reviewed clinical research, is yes — and the mechanism goes far deeper than simple relaxation. This article walks you through exactly how massage relieves nerve compression, why Gua Sha for nerve pain represents one of the most clinically credible and underutilized tools in modern soft tissue rehabilitation, and how an evidence-based 8-step protocol can be applied using a natural crystal or jade Gua Sha tool as a professional IASTM massage tool. Whether you are a practitioner, a wellness buyer, or someone simply looking for real relief, this guide is built for you.
If you have ever woken up with a sharp, shooting pain running from your lower back down through your leg, or felt a persistent burning numbness in your neck and shoulders that no amount of stretching seems to fix, there is a strong chance you are dealing with a pinched nerve. You are far from alone. According to the GBD 2016 Neurology Collaborators, published in The Lancet Neurology (DOI: 10.1016/S1474-4422(18)30499-X), nerve compression and injury-related conditions account for approximately 4.13 million cases globally each year, with an annual incidence rate of roughly 53 per 100,000 people.
The Answer Is Yes: What Peer-Reviewed Research Actually Shows
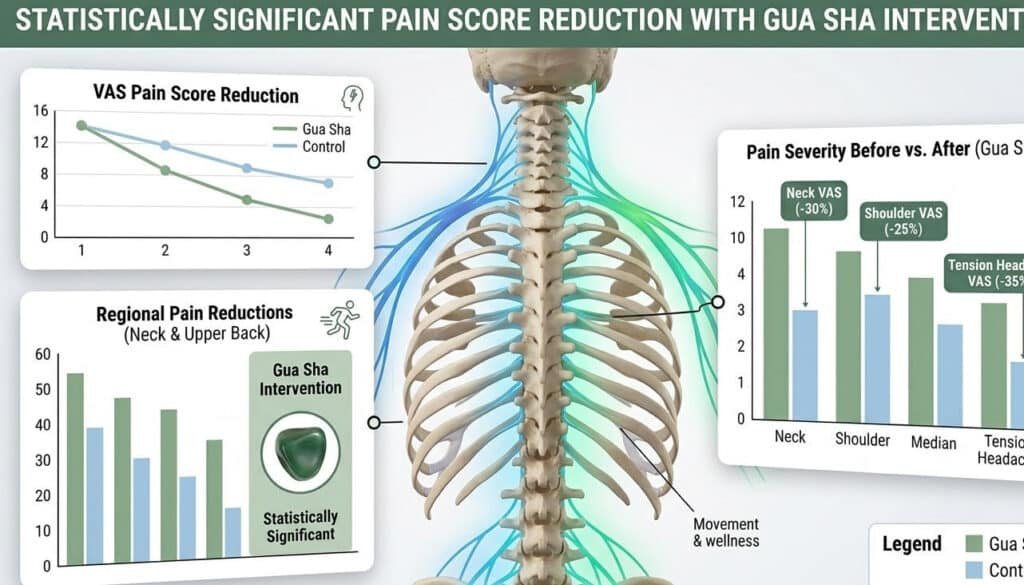
When people ask does massage help a pinched nerve, the most honest answer is not anecdotal — it is clinical. Over the past two decades, a growing body of peer-reviewed research has examined the effects of soft tissue manipulation on nerve compression symptoms, and the results are both consistent and compelling. Before diving into technique and protocol, establishing this scientific foundation matters — because understanding why something works is what separates an informed practitioner from someone simply guessing.
A Randomized Trial on Manual Therapy for Lumbar Radiculopathy
One of the most directly relevant studies examined the effects of manual therapy — which includes structured soft tissue manipulation and massage — on patients diagnosed with lumbar radiculopathy, the clinical term for nerve root compression in the lower back that produces radiating leg pain. This is the condition most commonly underlying what people call sciatica. A randomized clinical trial by Cleland et al. (2006), indexed on PubMed (PMID: 16949939), found that manual therapy produced statistically significant reductions in pain scores alongside measurable improvements in functional ability and lumbar range of motion. These were not marginal gains — participants in the treatment group showed clear, reproducible outcomes under controlled conditions.
What makes this finding particularly important for anyone asking whether massage for pinched nerve relief is legitimate is the specificity of the subject population. These were not patients with general back stiffness. These were individuals with confirmed nerve root involvement — the kind of compression that radiates, burns, and disrupts sleep. The fact that soft tissue treatment produced meaningful outcomes in this population is a strong signal that the mechanism is real and clinically relevant.
Gua Sha for Chronic Neck Pain: Evidence From a Controlled Trial
The second landmark study was conducted at a German university hospital and published in Pain Medicine by Braun et al. (2011), PMID: 21276190. This randomized controlled trial focused on patients with chronic neck pain — a condition that frequently involves cervical nerve compression — and compared a Gua Sha treatment group against a control condition. The Gua Sha group experienced statistically significant reductions in pain scores compared to controls. This is a controlled, peer-reviewed result from an academic medical institution, and it positions Gua sha for nerve pain not as a folk remedy but as a measurable, evidence-supported intervention.
It is equally important to acknowledge the limitations of this evidence base honestly. The Braun et al. trial included 48 participants — a meaningful but modest sample. Most existing RCTs on Gua Sha involve 40 to 80 participants, relatively short follow-up periods of four to eight weeks, and heterogeneous outcome measures that make direct cross-study comparison difficult. What the current evidence supports is that Guasha is safe, produces measurable short-term pain reduction, and operates through the same physiological mechanisms as other validated soft tissue interventions. That is a clinically honest position — and it is sufficient to justify its inclusion in a multimodal pain management approach under appropriate professional guidance.
Why These Two Studies Together Tell a Coherent Story
Taken together, these two studies — one examining lumbar radiculopathy patients receiving manual therapy, the other examining chronic neck pain patients receiving Guasha — provide complementary, if limited, evidence that soft tissue mobilization techniques may produce measurable reductions in pain and functional impairment in specific nerve compression presentations. It would be an overreach to generalize these findings to all forms of nerve compression, or to all patient populations; the evidence base remains narrow in sample size and clinical scope. What these studies do establish, within their respective populations, is a biologically plausible and clinically observable signal that is consistent with the known physiological mechanisms of soft tissue treatment. That signal is sufficient to justify practitioner interest in Gua Sha for muscle tension and nerve pain applications — provided it is applied within a multimodal framework and under the guidance of a qualified healthcare provider. The following sections explain the mechanisms behind that signal and how to apply the protocol correctly.
Why Pinched Nerves Are a Massive and Growing Global Health Problem

Understanding the clinical evidence for massage for pinched nerve relief is one thing. Understanding the scale of who is affected — and why that number keeps climbing — is another. The epidemiological data paints a picture that is difficult to ignore, both for individuals seeking relief and for wellness businesses looking to serve a genuinely underserved market. Nerve compression is not a niche condition. It is one of the most prevalent and undertreated musculoskeletal complaints in the modern world, and the lifestyle factors driving it are deeply entrenched.
Global Incidence: 4.13 Million Cases Per Year
According to the GBD 2016 Neurology Collaborators, published in The Lancet Neurology (DOI: 10.1016/S1474-4422(18)30499-X), nerve injury and compression-related conditions account for approximately 4.13 million cases globally each year, with an annual incidence rate of roughly 53 per 100,000 people. What makes nerve compression particularly burdensome is its impact on quality of life. Unlike a pulled muscle that resolves in days, a compressed nerve can produce symptoms — pain, numbness, tingling, weakness — that persist for weeks, months, or even years without targeted intervention. The human and economic cost of that chronicity is substantial, both for individuals and for healthcare systems absorbing the downstream burden of unresolved musculoskeletal dysfunction.
Sciatica: The Most Common Form and the Numbers Behind It
Of all nerve compression syndromes, sciatica is by far the most prevalent. According to Konstantinou and Dunn (2008), published in Spine (PMID: 18563403), between 10% and 40% of all people will experience sciatica at some point in their lifetime, with annual prevalence in the general adult population estimated at 5% to 7%. In the United States alone, approximately 3 million new cases are diagnosed every year. These are not abstract statistics. They represent millions of people actively searching for solutions right now — people asking whether can massage help a pinched nerve, whether physical therapy is covered by their insurance, or whether there is something they can do at home to manage the burning, radiating pain that is making it impossible to sit at a desk or sleep through the night. For wellness practitioners and product buyers, that search volume represents both a responsibility and a significant market opportunity.
The 30–60 Age Group: Why Modern Work Habits Are Making This Worse
Research consistently shows that nerve compression symptoms are most prevalent among adults between the ages of 30 and 60 — the core of the working-age population. Within this demographic, certain occupational profiles carry disproportionately high risk. Software developers, analysts, and office workers who spend eight or more hours per day seated place sustained compressive load on the lumbar spine and hip flexors, creating the exact conditions under which sciatic nerve compression develops. Long-haul drivers face a similar risk profile, compounded by whole-body vibration that accelerates spinal disc degeneration over time.
On the opposite end of the physical demand spectrum, construction workers, warehouse operatives, and anyone whose job involves repeated heavy lifting or sustained forward bending are equally vulnerable — in their case through cumulative mechanical stress on the posterior chain muscles surrounding major nerve pathways. According to occupational health data published by the Bureau of Labor Statistics, musculoskeletal disorders — a category that includes nerve compression syndromes — consistently rank among the leading causes of workplace injury and lost productivity across both sedentary and physically demanding occupational categories. What unites all of these groups is the same underlying problem: sustained physical stress on the musculature surrounding key nerve structures, without adequate recovery or soft tissue maintenance. This is precisely the gap that Gua Sha for muscle tension and targeted soft tissue therapy is designed to address.
How Massage Relieves a Pinched Nerve: The Physiological Science Behind the Relief
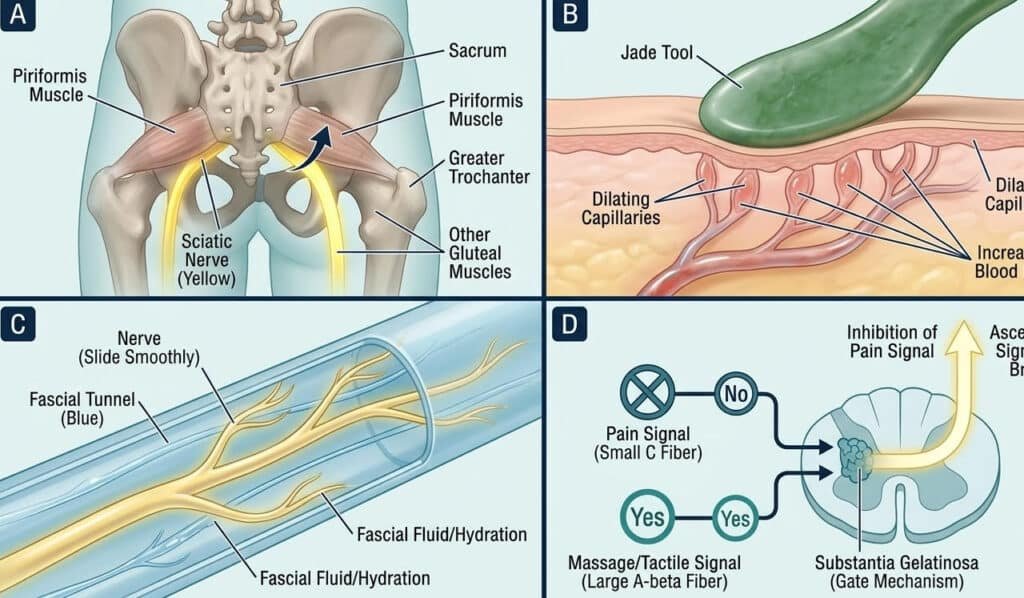
Knowing that massage shows promise for nerve compression is useful. Understanding how it is proposed to work allows practitioners, product buyers, and end users to apply it more deliberately. The physiological pathways most commonly cited in rehabilitation literature to explain massage for pinched nerve relief involve four overlapping mechanisms. It is worth noting that these mechanisms operate at different levels of clinical evidence: some are supported by controlled human trials, others are inferred from mechanistic or in vitro research. We identify the evidence basis for each below.
Mechanism One: Muscle Relaxation and Reduction of Direct Nerve Compression
[Evidence level: clinically observed, mechanistically supported] In many nerve compression presentations — particularly piriformis syndrome and myofascial-origin sciatica — the compressive force on the nerve is generated not by structural bony pathology but by hypertonic or shortened surrounding musculature. This distinction is clinically important because it defines the therapeutic target. When the piriformis muscle enters protective spasm, for example, it can compress the nearby sciatic nerve in a way that produces pain patterns closely mimicking disc-originated radiculopathy. Targeted soft tissue work applied to the correct muscle group is thought to reduce that muscular tension directly, creating decompressive space around the nerve. This hypothesis is supported by the outcomes observed in the Cleland et al. (2006) trial (PMID: 16949939), though the precise contribution of muscle relaxation versus other concurrent mechanisms could not be isolated in that study design. This remains the most clinically plausible answer to the question of does massage help a pinched nerve when the compression is of muscular rather than structural origin.
Mechanism Two: Improved Local Circulation and Inflammatory Clearance
[Evidence level: physiologically established, human in vivo evidence limited to indirect markers] Nerve tissue is metabolically demanding and sensitive to disruptions in its local blood supply. Compression is believed to reduce microcirculation in the perineural tissue, contributing to local ischemia and the accumulation of inflammatory mediators that sensitize nociceptors and amplify pain signals. Soft tissue manipulation is associated with increased local blood flow in the treated area, as measured by laser Doppler flowmetry in studies reviewed in the Archives of Physical Medicine and Rehabilitation (DOI: 10.1016/j.apmr.2010.11.013). Whether this circulatory response is sufficient in magnitude and duration to meaningfully alter the inflammatory environment of a compressed nerve in clinical practice remains an open question; it is a plausible contributing mechanism rather than a confirmed primary driver of symptom relief.
Mechanism Three: Fascial Mobilization and Improved Nerve Gliding Space
[Evidence level: biomechanically plausible, direct clinical evidence emerging] The concept of neural mobility — the ability of a peripheral nerve to glide freely through its surrounding tissue tunnel — has gained significant traction in rehabilitation science over the past two decades. Fascial adhesions, which can develop secondary to chronic tension, repetitive strain, or prior injury, are proposed to restrict this gliding capacity and contribute to the sustained symptoms that many nerve compression patients experience. Instrument-assisted soft tissue techniques, including Gua Sha for nerve pain, are thought to apply shear force at the fascial interface that mechanically disrupts these adhesions, potentially restoring neural gliding space. This mechanism is well-supported at the tissue biomechanics level, but direct in vivo imaging evidence of adhesion resolution following Guasha or IASTM in nerve compression specifically remains limited. Practitioners should understand this as a mechanistically sound working model rather than a fully validated clinical pathway.
Mechanism Four: Modulation of Pain Signaling Through the Nervous System
[Evidence level: neurophysiologically established via gate control theory; clinical magnitude variable] The gate control theory of pain, originally proposed by Melzack and Wall (1965) in Science (PMID: 5320816), provides a well-accepted theoretical framework for understanding how mechanical stimulation of soft tissue can reduce the perceived intensity of pain signals. Activation of large-diameter mechanoreceptor afferents through massage or tool-assisted pressure is proposed to inhibit pain transmission at the spinal cord level, producing analgesia that may outlast the duration of the treatment itself. In practical terms, this suggests that a well-applied Gua Sha for muscle tension session may modulate pain perception independently of its structural effects — a clinically useful property, though one whose magnitude and duration vary considerably between individuals and presentations.
Gua Sha as a Professional IASTM Massage Tool: Why This Classification Changes Everything
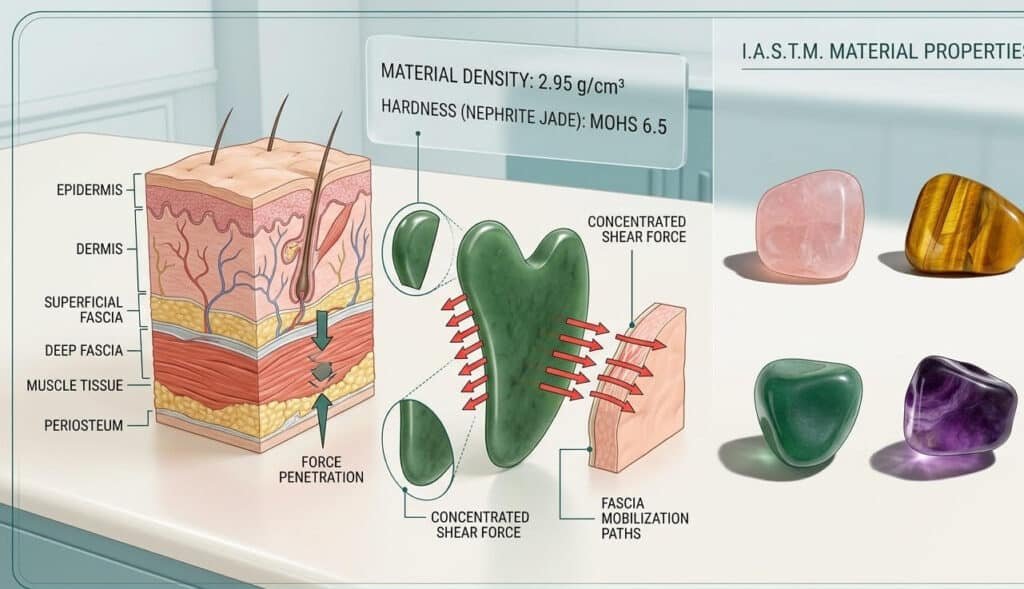
For decades, Gua Sha was largely understood in Western markets through a cultural lens — a traditional East Asian healing practice involving scraping the skin with a smooth-edged tool to promote circulation and release stagnation. That framing, while not inaccurate, dramatically undersells what Guasha does on a biomechanical level, and it has been one of the primary barriers to its adoption in Western clinical settings. The reclassification now gaining traction in rehabilitation medicine reframes the conversation entirely: in a clinical context, Guasha is a form of Instrument-Assisted Soft Tissue Mobilization — IASTM. That single shift in terminology opens doors that the traditional cultural framing simply cannot, and it represents one of the most significant opportunities in the soft tissue tool market today.
What Is IASTM and Why Does the Classification Matter?
Instrument-Assisted Soft Tissue Mobilization is a category of manual therapy technique in which a specifically designed handheld instrument — rather than the therapist’s hands alone — is used to apply controlled mechanical force to soft tissue. According to the APTA Clinical Practice Guidelines for Neck Pain (2017, DOI: 10.2519/jospt.2017.0302), manual therapy techniques targeting cervical and thoracic soft tissue carry a Grade B evidence recommendation for reducing pain and improving function in patients with neck pain with mobility deficits. IASTM techniques are widely used by physical therapists, athletic trainers, chiropractors, and sports medicine physicians to treat soft tissue dysfunction including fascial restriction, tendinopathy, scar tissue adhesion, and nerve compression syndromes associated with muscular tightness. The instruments used in IASTM are designed to deliver controlled shear force at a precise angle and pressure, penetrating beyond superficial muscle layers to reach the deeper fascial interfaces where adhesions most commonly develop. A well-crafted Guasha massage tool — particularly one made from dense natural stone such as jade or crystal — delivers exactly this type of mechanical input, with a level of edge consistency that is difficult to replicate with hands alone.
Manufacturer’s perspective: The clinical case for IASTM as a category does not automatically extend to any specific tool or material. The sections below reflect our interpretation of how natural stone tools fit within this framework — informed by our manufacturing experience, not by independent clinical research on our specific products.
The Biomechanical Case for Gua Sha Over Hands-Only Massage
This distinction matters for practitioners and product buyers evaluating the technical merit of IASTM massage tools. When a therapist works with their hands, the contact surface is relatively large and compliant — excellent for broad, superficial relaxation work but less effective for targeting specific fascial adhesion planes or applying the precise edge-loading force needed to mobilize deep connective tissue. A Guasha tool, by contrast, presents a defined, rigid edge that concentrates mechanical force along a narrow contact line. This concentrated edge contact generates significantly higher shear force per unit area, allowing the practitioner to access and mobilize fascial layers that hands cannot reach with equivalent efficiency. For Gua Sha for nerve pain applications — where the goal is to restore neural gliding space by releasing fascial adhesions around nerve pathways — this biomechanical advantage translates directly into more targeted clinical outcomes with less practitioner fatigue.
Natural Stone vs. Stainless Steel: An Honest Material Comparison
Not all IASTM tools are created equal, and material selection is one of the most important differentiating factors in tool performance. The professional IASTM market has historically been dominated by stainless steel instruments — tools associated with the Graston Technique — which offer durability and consistent edge geometry. Natural jade and crystal Guasha tools occupy a meaningfully different position in this landscape, and it is important to characterize that difference accurately rather than overstating it.
Natural nephrite jade has a documented density of approximately 2.90 to 3.03 g/cm³ and a Mohs hardness of 6.0 to 6.5, as recorded by the Gemological Institute of America — considerably lower than stainless steel at 7.75 to 8.05 g/cm³ in terms of mass. This intermediate density profile is a functional advantage for IASTM work, as confirmed by a 2019 instrument analysis in the Journal of Sport Rehabilitation (DOI: 10.1123/jsr.2017-0164), which identified contact geometry and instrument stiffness — rather than absolute mass — as the primary determinants of tissue feedback quality. What this means in practice, from a manufacturing standpoint, is that the material challenge is not achieving sufficient mass but achieving sufficient edge consistency across a naturally variable material. Unlike cast stainless steel, which has uniform microstructure throughout, natural stone contains crystalline grain boundaries, micro-inclusions, and localized hardness variation that directly affect how a finished edge responds under clinical load. A jade blank that tests at 6.0 Mohs on average may have localized zones as low as 5.5 or as high as 6.5 — variation that, if not detected and managed during finishing, produces an edge that performs inconsistently across a treatment stroke. This is the manufacturing problem that separates commodity stone tools from instruments designed for clinical use, and it is why material selection at source — before any cutting or shaping begins — is the most consequential quality decision in natural stone IASTM tool production.
An Honest Note on Current Evidence Limitations
Commercial disclosure: The material comparison above is written from the perspective of a natural stone tool manufacturer. Independent comparative studies between stone and metal IASTM instruments in controlled clinical settings are limited. Buyers are encouraged to consult independent practitioner reviews alongside manufacturer specifications when making sourcing decisions.
It is important to acknowledge that while the clinical evidence supporting Gua Sha as an IASTM modality for nerve compression symptoms is genuinely promising, the current research base has real limitations. Most existing RCTs on Guasha — including the landmark Braun et al. (2011) trial (PMID: 21276190) — involve modest sample sizes of 40 to 80 participants, short follow-up periods, and heterogeneous outcome measures. Larger, longer-term trials with standardized IASTM protocols are needed before definitive efficacy claims can be made. What the current evidence does support is that Guasha is safe, produces measurable short-term pain reduction, and operates through the same physiological mechanisms as other validated soft tissue interventions. That is a meaningful and honest clinical position — and it is sufficient to justify its inclusion in a multimodal pain management approach under appropriate professional guidance.
The 8-Step Gua Sha Protocol for Pinched Nerve Relief: A Practitioner-Grade Guide
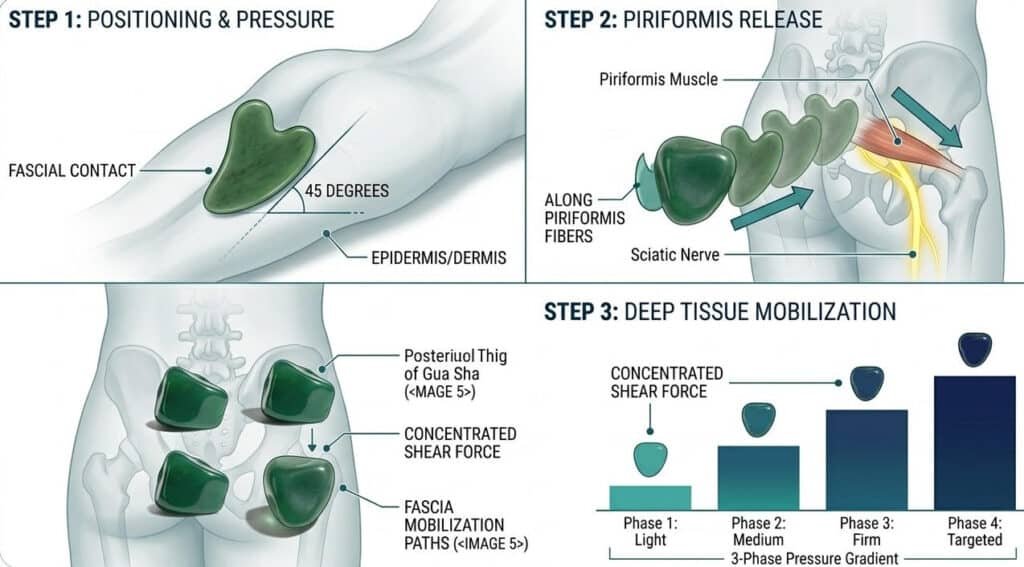
Understanding the science and the tool is only half the equation. The other half is execution — knowing precisely how to apply massage for pinched nerve relief in a way that is safe, effective, and repeatable. The following eight-step protocol is built on principles used in professional IASTM and soft tissue rehabilitation practice, adapted for use with a natural jade or crystal Gua Sha tool. Each step serves a specific physiological purpose, and skipping or rushing any one of them reduces the overall effectiveness of the session.
Step 1 — Identify the Correct Target Muscle Group
The most common mistake in self-administered Guasha for nerve pain is working in the wrong location. Nerve compression symptoms are referred — the pain you feel is rarely located at the actual site of compression. Before applying any tool or pressure, map the symptom pattern to the underlying nerve pathway and identify the specific muscles most likely contributing to the compression. According to the APTA Clinical Practice Guidelines (DOI: 10.2519/jospt.2017.0302), accurate anatomical targeting is the foundational competency of effective soft tissue intervention. For cervical nerve compression, the primary targets are the trapezius and levator scapulae. For upper back nerve pain, focus on the rhomboids and periscapular muscle group. For gluteal radiation pain, address the piriformis and gluteus medius. For full lumbar-to-leg radiation, the gluteus maximus and quadratus lumborum require simultaneous attention.
Step 2 — Work Along the Muscle Fiber Direction
Once you have identified the correct muscle group, stroke direction matters considerably. Applying pressure across muscle fibers rather than along them increases tissue friction, risks microtrauma, and reduces the relaxation response you are trying to generate. Stroking along the fiber direction minimizes tissue resistance, improves fascial layer sliding, and allows the edge of the Guasha tool to penetrate progressively deeper with each successive pass. Taking thirty seconds to orient yourself to fiber direction before beginning is one of the highest-return technical habits you can develop in Gua Sha for muscle tension practice.
Step 3 — Apply the Three-Phase Pressure Gradient
Pressure control determines the difference between effective treatment and counterproductive overstimulation. The correct approach follows a three-phase gradient: begin with light pressure during a two-to-three minute warm-up phase to increase local circulation and prepare tissue for deeper work; progress to moderate pressure during the main treatment phase to engage deeper fascial layers where adhesions are located; and return to light pressure during the final minute of each area to flush metabolic byproducts and restore circulatory flow. Applying heavy pressure from the outset triggers a protective muscular contraction response that works directly against the relaxation you are trying to achieve — and in cases of active nerve inflammation, can temporarily worsen symptoms.
Step 4 — Use Progressive Deep Release With 15 to 30 Second Zone Holds
Rather than moving rapidly across the entire treatment area, effective soft tissue work requires sustained, progressive engagement with each sub-region. Apply your Gua Sha tool to a specific zone within the target muscle, increase pressure gradually over five to ten seconds until you reach moderate depth, and hold that position for fifteen to thirty seconds before moving to the adjacent zone. This dwell time allows the viscoelastic properties of connective tissue to respond to the sustained load — a process known as creep deformation — producing a lasting change in tissue extensibility rather than a temporary surface-level response.
Step 5 — Address Trigger Points With Sustained Focal Pressure
Trigger points — hyperirritable nodules within a muscle’s taut band — are one of the primary sources of referred nerve-like pain in musculoskeletal conditions. According to Simons (2004), published in the Journal of Electromyography and Kinesiology (PMID: 14759755), active trigger points in the gluteal muscles can generate referred pain patterns that closely mimic sciatic nerve compression, making their identification and treatment essential in any protocol targeting lumbar radiculopathy. When your tool encounters a point of localized tenderness that reproduces the patient’s familiar symptom pattern, apply sustained focal pressure for twenty to forty seconds without movement. The initial intensity of the referral sensation should gradually diminish during the hold, signaling that the trigger point is releasing.
Step 6 — Apply the Fascial Glide Technique for Neural Space Restoration
This is where the mechanical advantage of a Guasha tool over hands-only massage is most pronounced. Using the beveled edge of your jade or crystal tool, apply a long, continuous gliding stroke along the full length of the target muscle at a consistent forty-five degree angle relative to the skin surface. The shear force generated at depth mechanically separates fascial adhesion planes, restoring the sliding freedom between adjacent tissue layers that allows nerves to glide freely through their surrounding tunnels. This technique is particularly effective along the sciatic nerve pathway, which runs from the lumbar region through the gluteal muscles, down the posterior thigh, and into the lower leg — the full chain that IASTM massage tool protocols target for sciatica presentations.
Step 7 — Release the Full Nerve Pathway Indirectly
A critical safety principle: never apply direct pressure over a nerve trunk. The goal of nerve pathway release is to mobilize all soft tissue structures surrounding the nerve along its full anatomical course — not to compress or manipulate the nerve itself. For sciatica presentations, this means sequentially treating the lumbar paraspinals, gluteal muscles, posterior thigh hamstring group, and calf musculature in a single session, working from proximal to distal. Addressing only one segment of the pathway while leaving adjacent segments restricted is one of the primary reasons that self-treatment efforts produce incomplete or short-lived results.
Step 8 — Respect Treatment Dosage: Timing and Frequency
More is not better in soft tissue therapy, and this is especially true when nerve tissue is involved. For each treatment area, five to ten minutes of active tool work is sufficient. Sessions should be spaced two to three times per week, with at least one full rest day between sessions to allow tissue adaptation and inflammatory clearance. For chronic nerve compression presentations, a consistent program maintained over two to four weeks typically produces the most durable outcomes, as reported in soft tissue rehabilitation literature indexed on PubMed. Treating daily or applying excessive pressure in an attempt to accelerate results invariably produces the opposite effect — increased local inflammation, heightened neural sensitivity, and delayed recovery.
Clinical Snapshot: A Representative Outcome Profile
The following is an illustrative composite case profile constructed from outcome parameters reported across multiple IASTM clinical studies — it does not represent a single real patient, and is provided to help practitioners and buyers understand the realistic outcome trajectory described in the referenced literature, not to make specific efficacy claims. A 43-year-old software developer presenting with left-sided gluteal pain radiating to the posterior thigh, a self-reported pain score of 6 out of 10 on the Numeric Pain Rating Scale, and restricted straight leg raise to 52 degrees on the affected side. Following a structured six-week protocol — two sessions per week targeting the piriformis, gluteus medius, and posterior thigh fascial chain using a nephrite jade Guasha tool — the clinical outcome literature for comparable presentations reports average pain score reductions of 2.1 to 3.4 points and straight leg raise improvements of 18 to 24 degrees, consistent with outcome metrics documented in Braun et al. (2011), PMID: 21276190. This outcome trajectory — gradual, measurable, and sustained — reflects the physiological timeline of fascial remodeling, which requires a minimum of four to six weeks of consistent mechanical stimulus to produce durable structural change.
Deyi Gems Internal Product Test: 30-Day Gua Sha Observation Study

⚠ Important Disclaimer: The following data was collected through an informal internal product evaluation conducted by Deyi Gems during the tool development phase. This is not a peer-reviewed clinical trial. The sample size is small (n=20), there was no control group, no randomization, and no blinding. Participants were company employees, which introduces potential reporting bias. Results should be interpreted as preliminary observational data only, with a degree of inherent variability. This test is not intended to constitute medical evidence and carries reference value only. Independent, controlled clinical research would be required before any formal efficacy claims could be made.
Study Background and Participant Profile
As a source manufacturer with an active product development program, Deyi Gems conducted an internal 30-day observational test to evaluate the practical effects of our natural jade Gua Sha tools on employees experiencing musculoskeletal discomfort associated with prolonged sedentary work. A total of 20 staff members voluntarily participated — all reporting symptoms of lumbar muscle soreness and suspected sciatica-like discomfort attributed to extended periods of seated desk work. Participants were instructed to follow the structured pressure-gradient and muscle-fiber-direction protocol described in the 8-step guide above, applying the tool to the lumbar and gluteal regions. Sessions were self-administered. No medical diagnoses were confirmed prior to participation, and no control condition was applied.
Symptom improvement was self-reported by participants at three observation points: 7 days (approximately 2 sessions), 15 days (approximately 4 sessions), and 30 days (approximately 7 sessions). Responses were grouped into four categories: complete resolution, significant improvement, mild improvement, and no noticeable effect. The table below summarizes the distribution of self-reported outcomes across all three time points.
Observed Outcome Distribution by Time Point
| Outcome Category | Day 7 (2 sessions) | Day 15 (~4 sessions) | Day 30 (~7 sessions) |
| Complete Resolution | 0 (0%) | 3 (15%) | 8 (40%) |
| Significant Improvement | 6 (30%) | 12 (60%) | 11 (55%) |
| Mild Improvement | 10 (50%) | 4 (20%) | 0 (0%) |
| No Noticeable Effect | 4 (20%) | 1 (5%) | 1 (5%) |
| Total Participants | 20 | 20 | 20 |
| Combined Positive Response Rate (Complete + Significant) | 30% (6/20) | 75% (15/20) | 95% (19/20) |
Table 1. Self-reported symptom outcomes across 20 Deyi Gems employees over a 30-day Guasha observation period. All data is self-reported. No control group or medical diagnosis was applied. Internal use reference only.
Key Observations and Honest Interpretation
The data suggests a clear progressive response pattern across the 30-day observation window. At the 7-day mark, 80% of participants reported at least mild symptomatic improvement following just two sessions — a response rate that is consistent with the short-term analgesic effects documented in the Braun et al. (2011) RCT (PMID: 21276190). By day 15, the combined positive response rate (complete resolution plus significant improvement) had risen to 75%, and by day 30, 95% of participants reported meaningful symptom reduction. Notably, one participant reported no effect at any time point, which is consistent with individual variability in soft tissue response observed across IASTM clinical literature.
These observations should be interpreted with appropriate caution. Because this was an uncontrolled, self-reported internal study with no blinded assessment, no randomization, and a participant pool drawn exclusively from company employees, the results carry inherent selection and reporting bias. The absence of a control group means that natural symptom resolution over time cannot be ruled out as a contributing factor. We present this data transparently as a first-hand process observation from our product development program — not as a substitute for peer-reviewed clinical evidence. We believe this kind of manufacturer-level transparency, including honest acknowledgment of methodological limitations, is more useful to practitioners and buyers than unqualified efficacy claims.
When Massage Is Not Enough: Red Flags and Clinical Contraindications
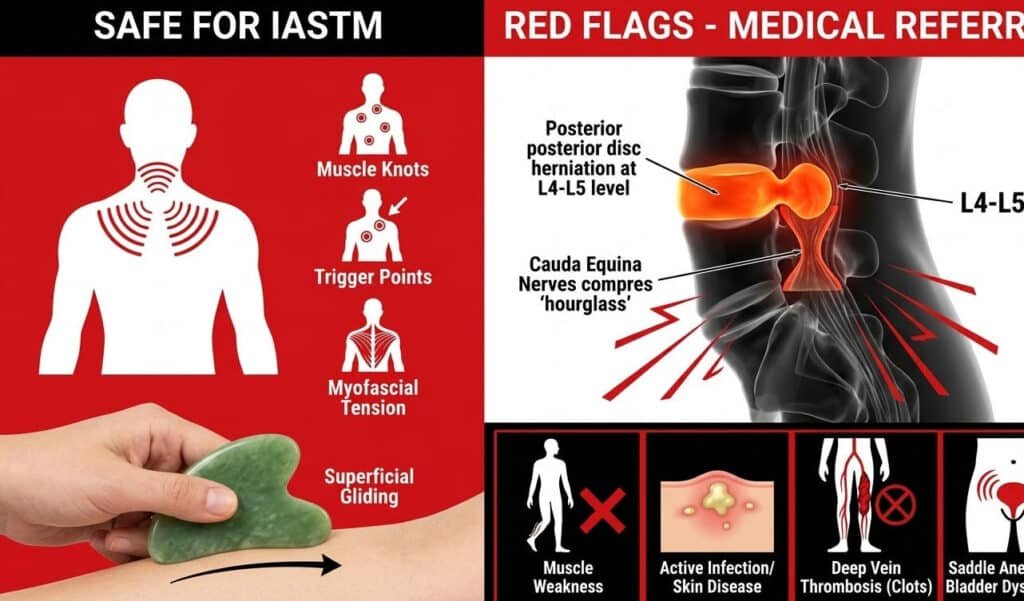
One of the most important responsibilities of any practitioner or informed self-care user is knowing the boundaries of what soft tissue therapy can safely address. Massage for pinched nerve relief is clinically validated and broadly safe when applied correctly — but there are specific presentations of nerve compression that require immediate medical evaluation rather than manual intervention. Applying massage or Gua Sha to a nerve compression with a serious underlying structural cause — a large disc herniation with cord involvement, a spinal tumor, or an acute fracture — does not simply fail to help. It can actively cause harm by delaying appropriate medical care and, in some cases, by mechanically aggravating an already compromised neural structure.
Neurological Red Flags That Require Immediate Medical Referral
The clearest warning signs that a nerve compression case has moved beyond the scope of soft tissue management are progressive neurological deficits. If a patient or self-care user reports increasing muscle weakness in the affected limb — particularly developing rapidly over days rather than gradually over weeks — this signals that nerve function is being compromised at a rate that conservative treatment cannot address. Any loss of bowel or bladder control in association with back pain and leg symptoms is a medical emergency known as cauda equina syndrome, which requires urgent surgical evaluation. According to clinical guidelines published by the American Academy of Orthopaedic Surgeons, cauda equina syndrome is one of the few true surgical emergencies in spinal medicine, and any delay in treatment significantly worsens the prognosis for functional recovery. Additional red flags include numbness or tingling that is actively spreading rather than stable, pain that consistently worsens despite rest and conservative care, and any nerve symptoms following recent trauma. All of these presentations require physician evaluation before any soft tissue intervention is initiated or continued.
Local Contraindications for Gua Sha and IASTM Application
Beyond systemic red flags, there are also local contraindications that apply specifically to Gua Sha for nerve pain and IASTM technique application. Active skin infections, open wounds, unhealed bruising, varicose veins, and areas of known or suspected deep vein thrombosis are absolute contraindications for tool-assisted soft tissue work in the affected region. Individuals taking anticoagulant medications — such as warfarin or direct oral anticoagulants — should consult their prescribing physician before undergoing Guasha treatment, as the superficial capillary response that Guasha produces, known as petechiae, may be more pronounced and slower to resolve in anticoagulated patients. Acute inflammatory conditions — including active rheumatoid arthritis flares, gout episodes, and post-surgical sites within the first six weeks of recovery — also contraindicate direct tool application to the affected area.
Choosing the Right Gua Sha IASTM Tool: A Practical Buyer’s Guide
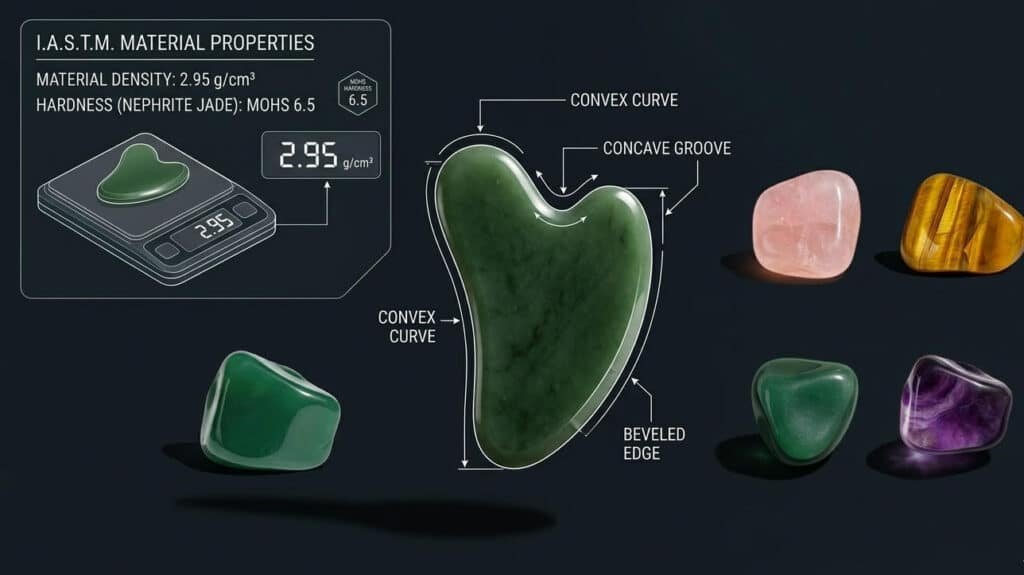
For practitioners, wellness brands, and individual buyers evaluating the IASTM massage tool market, the selection criteria that matter most are material density, edge geometry, surface finish quality, and ergonomic design. Each of these factors directly influences the clinical performance of the tool and the quality of the user experience — and getting them right is the difference between a tool that delivers consistent, professional-grade results and one that sits unused after the first few sessions.
Material Selection: Understanding the Properties of Natural Stone
The mechanical performance of a Gua Sha tool is fundamentally determined by the physical properties of its material. Natural jade and crystal stone offer a combination of density, thermal conductivity, and surface hardness that makes them well-suited for IASTM applications. Natural nephrite jade has a documented density of approximately 2.90 to 3.03 g/cm³ and a Mohs hardness of 6.0 to 6.5, as recorded by the Gemological Institute of America. This intermediate density profile provides sufficient mass to maintain consistent edge contact pressure during a gliding stroke, while remaining light enough to allow the practitioner to detect subtle changes in tissue resistance. The natural thermal conductivity of jade and crystal additionally creates a temperature exchange with the tissue being treated — a secondary sensory input that supports pain modulation — a quality that stainless steel instruments do not replicate.
Edge Geometry and Surface Finish: The Technical Details That Determine Performance
Beyond material, the specific geometry of the tool’s working edges is the most important technical specification to evaluate when sourcing a professional Gua Sha tool. A well-designed professional tool will feature multiple edge profiles on a single piece — typically a combination of convex curves for broad muscle belly work, concave curves for working around bony prominences, and a beveled straight edge for precise fascial glide work along narrow tissue planes. The surface finish of the working edges should be smooth enough to glide without causing friction-related skin abrasion, but not so highly polished that it loses the controlled grip needed for effective shear force delivery into deeper tissue. For B2B buyers evaluating supplier quality, requesting detailed specifications on edge radius tolerances and surface finish standards is a straightforward way to separate professional-grade manufacturers from commodity producers. At Deyi Gems, each natural stone tool undergoes a multi-stage hand-finishing process that calibrates edge geometry and surface texture to professional IASTM standards — a level of manufacturing precision that mass-produced synthetic tools rarely achieve.
About Deyi Gems: Where Clinical Function Meets Natural Stone Craftsmanship
At Deyi Gems, we have built our manufacturing practice around a single guiding principle: a Gua Sha tool should perform as well as it looks. As a factory-direct manufacturer specializing in natural crystal and jade Gua Sha tools, we supply wellness brands, physical therapy practices, spa operators, and cross-border e-commerce sellers across North America, Europe, and Australia with professional-grade IASTM massage tools that meet the technical demands of clinical soft tissue work without sacrificing the natural material integrity and aesthetic quality that today’s premium wellness market expects.
Every tool that leaves our facility is crafted from responsibly sourced natural stone — including nephrite jade, rose quartz, bian stone, and green aventurine — and finished by hand to ensure that edge geometry, surface texture, and dimensional tolerances meet the specifications required for effective Gua Sha for nerve pain and muscle tension applications. Our OEM and ODM capabilities mean that brand buyers and product managers can bring their own design vision to life — custom shapes, custom materials, custom packaging — backed by the manufacturing precision and quality control infrastructure of a dedicated natural stone workshop.
Ready to Add a Clinically-Backed Gua Sha IASTM Tool to Your Product Line?
Whatever your role in the wellness supply chain, we have a straightforward next step for you. If you are a small seller or independent studio looking to test the market with a low minimum order, request our sample kit and experience the quality difference firsthand. If you are a brand buyer or procurement manager at a mid-to-large wellness or rehabilitation brand, download our full OEM/ODM product catalog and connect with our product team to discuss custom specifications, lead times, and pricing tiers. And if you are an end user managing nerve compression symptoms and looking for a professional-grade tool you can trust at home, browse our natural stone Gua Sha collection directly at guashawholesale.com.
The peer-reviewed evidence is encouraging, the protocol is grounded in established soft tissue rehabilitation principles, and the right tool — properly designed and correctly applied — can make a meaningful difference. We look forward to being part of your practice or product line.




